Let’s Talk about HPV
Overview & Introduction
When it comes to our health, knowledge really is power - especially when it comes to something as common and important as HPV.
Many people feel uneasy or unsure when they hear about human papillomavirus, and that’s completely understandable. But here’s the reassuring truth: while HPV is widespread, it doesn’t have to be scary. With the right information, regular screening, and preventative care, you can stay informed, stay protected, and take control of your long-term health.
Let’s break down what HPV is, why it matters, and the steps you can take to look after yourself.
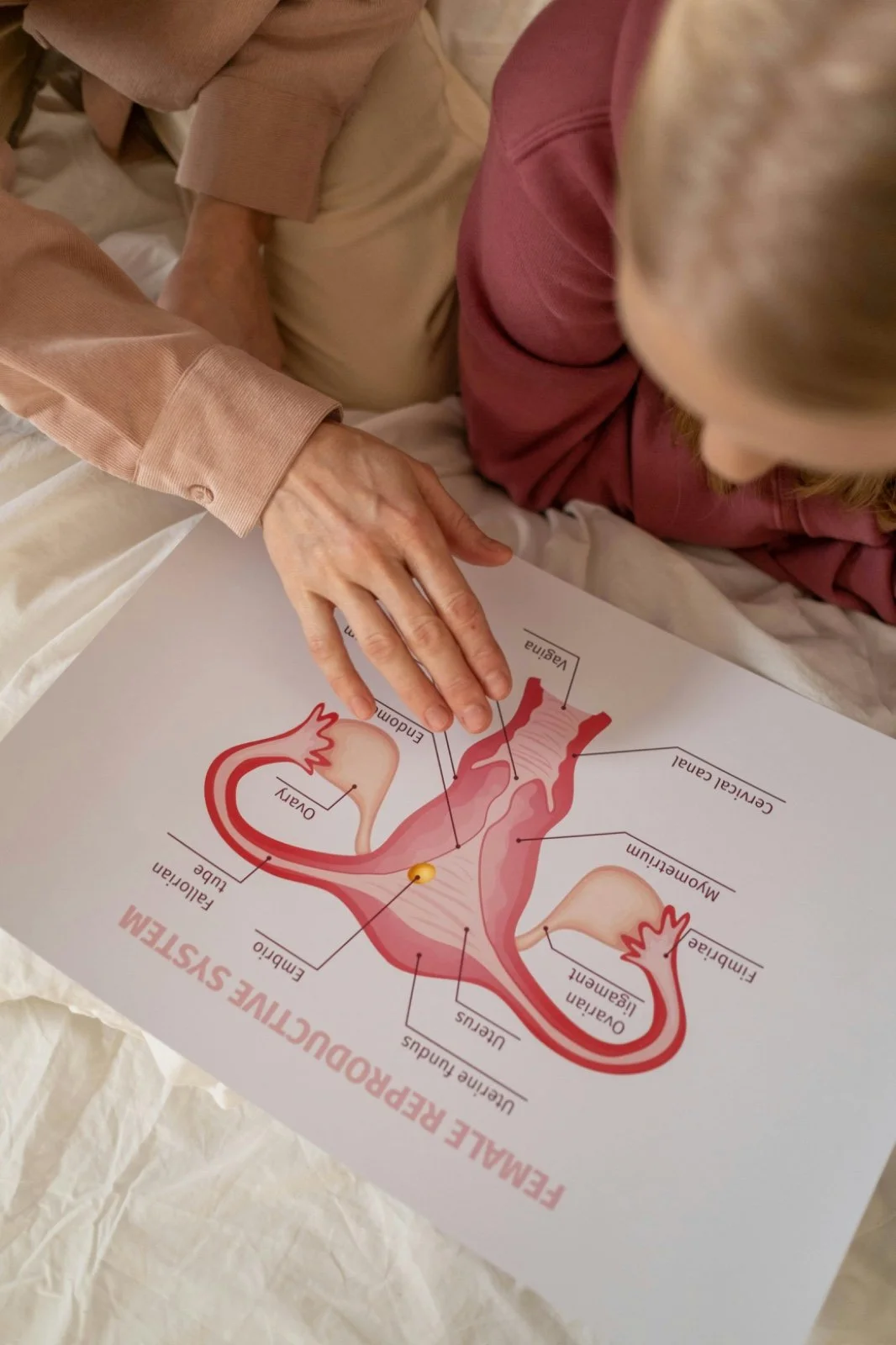
What Is HPV?
Human papillomavirus, more commonly known as HPV, refers to a group of more than 100 related viruses. These viruses are incredibly common and are primarily spread through intimate skin-to-skin contact. In fact, most individuals engaging in intimacy will come into contact with HPV at some point in their lives, often without even knowing it.
In many cases, with a strong and healthy immune system, the body can naturally clear the virus without causing any harm. However, certain types of high-risk HPV can persist and are associated with serious health-related conditions such as vulval, vaginal, and most commonly cervical cancer.
HPV is one of the most common sexually-transmitted infections worldwide - and South Africa is no exception. Studies suggest that the incidence of HPV in South Africa was three-times the global rate in 2020, and it was the leading cause of female cancer deaths in those aged 15-44 years. This is why we chose to demystify this common, and potentially devastating condition.
Different Types of HPV
HPV is generally divided into two main categories:
Low-risk HPV types (HPV 6, 11 and others)
These types are not associated with cancer but often cause conditions like genital warts. While these may be uncomfortable or distressing, they are typically manageable and not life-threatening.
High-risk HPV types (HPV 16, 18 and others)
Types like HPV 16 and 18 are considered high-risk because they are linked to cervical cancer. Persistent viral infection with high-risk HPV genotypes causes nearly all cervical cancers with around 65% of all invasive cervical cancers being attributed to HPV 16 or 18. Thus, high-risk types require more urgent attention, and the prevention of invasive cervical cancer includes early detection of HPV, and if positive cervical screening.
How Does HPV Present?
Some possible presentations include:
No symptoms at all (the most common scenario - as HPV can remain dormant or latent for many years)
Genital warts, which may appear as small flesh-coloured bumps or clusters in the genital area
Cell changes in the cervix, which may present as an abnormal discharge, abnormal bleeding - including bleeding after intercourse, or lower abdominal pain. Very early changes cannot be seen or felt but can be detected through screening
Why Screening Matters
Early HPV detection and cervical screening is one of the most effective tools we have to prevent cervical cancer.
Rather than waiting for symptoms to appear, screening allows us to detect HPV and identify early cell changes long before they become serious. When caught early, these changes can be monitored or treated effectively.
The World Health Organization and newer research now recommends HPV DNA testing as the preferred screening method, as it is simple and cost-effective. A negative HPV test infers and reassures that you are at low-risk of developing pre-malignant cervical changes.
Given the higher rates of cervical cancer in South Africa, regular screening is especially important. Quite simply, early detection saves lives.
At Bowwood Family Practice, we follow evidence-based guidelines and offer:
HPV DNA testing
Liquid-based cytology - if HPV results are positive, if you have never had a previous Pap smear, or if there are any concerns that warrant further investigation
HPV self-testing kits for added convenience and comfort
We aim to make screening as accessible and supportive as possible.
When Should You Get Screened?
General guidelines recommend that women begin cervical screening from the age of 25, until approximately 60 years of age. The recommended screening interval is between 5-10 years when using HPV DNA testing, but this interval can vary depending on individual risk profile, previous test results and resources.
If you’re unsure when you last had a screening - or if you’ve never had one - this is a great opportunity to start the conversation. We’re here to guide you through it.
What about the HPV vaccine?
The HPV vaccine is another powerful way to protect your health.
South Africa introduced a school-based vaccination programme in 2014, helping to protect younger generations early on. The vaccine is most effective before exposure to HPV (usually in adolescence), but adults can still benefit - especially as it may protect against strains you haven’t yet encountered.
The most commonly available vaccines locally are Gardasil and Cervarix. Gardasil offers broader protection, covering strains linked to both cervical cancer and genital warts.
It’s important to keep in mind:
Even if you’ve been vaccinated, regular screening is still essential. The vaccine protects against the most common high-risk types - but not all of them.
The bottom line
HPV is common - but the complications and sequelae of it is largely preventable.
With regular screening, vaccination, and a proactive approach to your health, you can significantly reduce your risk. It’s not just about a test - it’s about taking care of your future self.
If you’ve been putting off your screening, consider this your gentle nudge. And if you have any questions or concerns, we’re always here to support you in a warm, respectful and non-judgmental space.
Your health matters. Let’s take care of it, together.
Warmest,
Drs Robynne Glasser & Lauren Goliath